|
hr -1) calcium-chloride continuous intravenous administration in seven patients (78%) with documented preoperative hypocalcemia.The hypocalcemia was severe (<3.0 mg/dl) and responded poorly to high-dose (10-15 mg All patients showed significant (<4.0 mg/dl) hypocalcemia in the immediate postoperative period. Additional complications were pericardial effusion requiring surgical drainage (one patient), chylothorax requiring chest tube insertion (one patient), and Pseudomonas aeruginosa pneumonia treated with cephalosporin and aminoglycoside antibiotics (one patient). The causes of respiratory insufficiency in these patients included vocal cord granuloma necessitating treatment by laser (one patient), preexisting bilateral phrenic nerve palsy palliated with surgical plication of the right hemidiaphragm (one patient), and bronchopulmonary dysplasia in one patient, who was operated on initially as a premature, 2.1 kg neonate. Three patients, however, had prolonged respiratory failure necessitating 2 to 6 weeks of mechanical ventilation. Ventilatory support need ranged from 4 to 7 days in most patients (78% Table III). No superficial or deep wound infections were observed in our series. (J Thorac Cardiovasc Surg 1996 111:348-58)įor all patients, the closure of the sternum was completed in the intensive care unit 1 to 5 days (median 2 days) after the original surgical procedure. Conclusions: Relief of severe subaortic stenosis during one-stage neonatal repair of aortic arch interruption and ventricular septal defect can be accomplished successfully without resection of the conal septum. Growth of the subaortic region was demonstrated in all patients (mean ratio of subaortic to descending aortic diameter, 1.20 ± 0.10 <0.001). 
On follow-up echocardiography (1 to 29 months, median 12 months), no patients had significant residual subaortic obstruction and one patient had mild residual arch obstruction (20 mm Hg). Median intensive care unit and hospital stays were 17 days (6 to 47 days) and 21 days (10 to 55 days), respectively. With a transpulmonary (seven patients) or transatrial (two patients) approach and without resection of the conal septum, the ventricular septal patch was placed on the left side of the septum to deflect the conal septum anteriorly and away from the subaortic area. All patients had severe subaortic stenosis according to preoperative echocardiography (mean ratio of subaortic to descending aortic diameter, 0.63 ± 0.08). 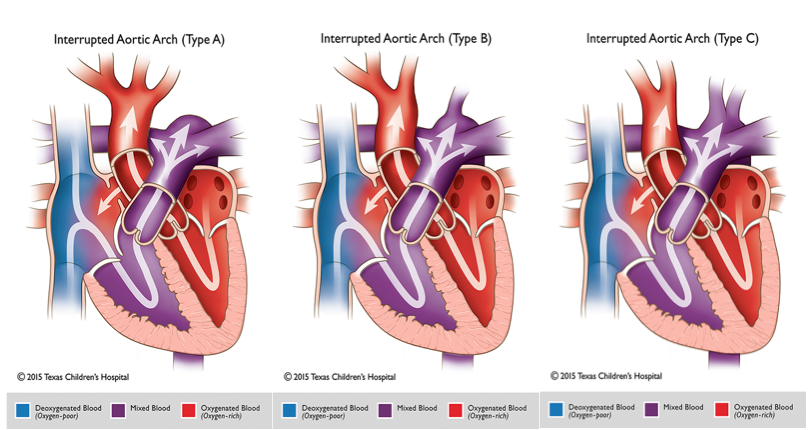
Methods and results: A new operative approach was used in nine neonates (2.1 to 3.9 kg) who underwent one-stage repair of interrupted aortic arch (type B, eight patients type C, one patient), ventricular septal defect, and severe subaortic stenosis. Techniques that use extracardiac conduits to bypass the subaortic area or involve transaortic or transatrial resection of the conal septum have shown limitations and have failed to reduce the high mortality rate associated with subaortic obstruction. Background: One-stage repair of interrupted aortic arch, ventricular septal defect, and severe subaortic stenosis represents a surgical challenge.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
